Antimicrobial resistance is one of the most pressing health threats facing the world today. But what exactly is antimicrobial resistance—and why is it such a big deal? Simply put, antimicrobial resistance (AMR) occurs when microorganisms like bacteria, viruses, fungi, and parasites adapt in ways that render drugs—such as antibiotics, antivirals, or antifungals—ineffective. As a result, infections that were once easily treatable become difficult or even impossible to cure.
This emerging crisis has wide-reaching implications. Not only does it put lives at risk, but it also threatens the foundations of modern medicine, from routine surgeries and cancer treatments to childbirth and organ transplants. Without effective antimicrobials, we risk returning to a time when even minor infections could be deadly.
The Global Impact of Antimicrobial Resistance
Antimicrobial resistance is already responsible for millions of deaths worldwide. In 2019 alone, AMR directly caused an estimated 1.27 million deaths and contributed to nearly 5 million more. If left unchecked, projections suggest that by 2050, drug-resistant infections could kill up to 10 million people every year.
Beyond the devastating human toll, AMR also carries severe economic consequences. Experts estimate that the global economy could lose up to $100 trillion by 2050 due to productivity losses, increased healthcare costs, and reduced workforce participation. Countries with fragile healthcare systems, especially in parts of Sub-Saharan Africa, South Asia, and Southeast Asia, are expected to bear the brunt of this crisis.
How Does Antimicrobial Resistance Develop?
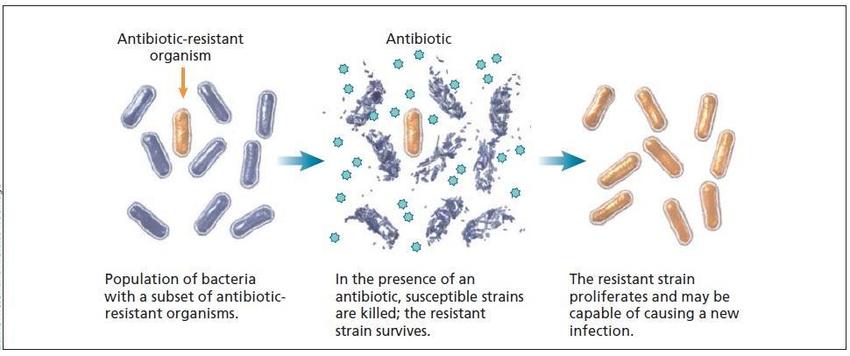
Antimicrobial resistance is a natural phenomenon, but human activity has accelerated the process dramatically. Resistance typically occurs when microorganisms undergo genetic changes that enable them to survive exposure to a drug. Over time, these resistant strains multiply, spread, and become dominant.
Several key factors contribute to the rise of AMR:
- Overuse and misuse of antibiotics: Taking antibiotics for viral infections (like the common cold or flu), or using them without a proper diagnosis, can fuel resistance.
- Incomplete treatment courses: Stopping antibiotics too early allows surviving microbes to regroup and develop resistance.
- Over-the-counter availability: In many regions, people can buy antibiotics without a prescription, leading to misuse.
- Use in agriculture: Antibiotics are frequently given to animals for growth promotion or disease prevention, even when not necessary.
- Environmental contamination: Pharmaceutical waste, hospital runoff, and agricultural discharge often release antimicrobials into the environment, creating hotspots for resistant microbes to evolve.
Together, these practices have created a global situation where once-effective drugs are now failing at an alarming rate.
Spotlight on Nigeria: Leading the Fight Against AMR
Nigeria is one of the countries facing a rapidly intensifying antimicrobial resistance crisis. In response, the Nigerian National Antimicrobial Stewardship Taskforce (NNAST) was established to lead a coordinated national response.
NNAST’s mission is to ensure antimicrobials are used appropriately and responsibly across human, animal, and environmental sectors. The taskforce operates under a One Health framework—recognizing that the health of people, animals, and the environment are closely interconnected.
Some of NNAST’s key strategies include:
- Implementing antimicrobial stewardship programs in hospitals and pharmacies
- Strengthening surveillance systems to track resistance trends
- Updating national treatment guidelines based on local data
- Promoting community education and awareness around appropriate antimicrobial use
- Encouraging research and innovation in alternative treatments and diagnostics
By addressing AMR through a collaborative and evidence-based approach, NNAST is helping Nigeria take meaningful steps toward containing and reversing the crisis.
A Global Effort: One Health and International Collaboration
Antimicrobial resistance is not just a national issue—it’s a global one. International organizations have adopted the One Health approach to tackle AMR, which means integrating human health, veterinary care, and environmental management into a single strategy.
The World Health Organization (WHO) and its partners have launched a Global Action Plan to help countries build robust AMR surveillance systems, promote responsible drug use, and encourage the development of new treatments.
Globally, antimicrobial stewardship is a cornerstone of these efforts. It emphasizes using the right antimicrobial, at the right dose, for the right duration, and only when necessary. This ensures that drugs are effective for as long as possible while minimizing the emergence of resistance.
Innovation and the Need for New Solutions
A major challenge in the fight against antimicrobial resistance is the slow pace of innovation. Since the discovery of penicillin, only a few new classes of antibiotics have been developed—and none since the late 1980s. This has left the medical community reliant on a limited number of drugs, many of which are now losing their effectiveness.
To address this, scientists and researchers are exploring new frontiers, including:
- Antimicrobial peptides designed to kill bacteria without resistance
- Phage therapy, which uses viruses to target and destroy bacteria
- CRISPR-based gene editing to disable resistance genes
- Vaccines to prevent infections before they require antimicrobial treatment
- Artificial intelligence to identify new drug candidates faster
- Photodynamic therapy and nanoparticle systems to combat drug-resistant biofilms
Additionally, governments are being urged to create better financial incentives for pharmaceutical companies to invest in antibiotic research and development. Without this support, the antibiotic pipeline will remain dangerously dry.
What Can You Do to Combat Antimicrobial Resistance?
While systemic change is essential, individual actions also make a significant impact in the fight against AMR. Here’s how you can help:
- Only use antibiotics when prescribed by a qualified healthcare professional.
- Complete the full course of treatment, even if you feel better before it ends.
- Never share or save antibiotics for future use.
- Avoid self-medicating or using leftover drugs from previous illnesses.
- Practice good hygiene, including handwashing, food safety, and proper sanitation.
- Get vaccinated to reduce your risk of infection and reliance on antimicrobials.
- Spread awareness—talk to family and friends about the dangers of antibiotic misuse.
These everyday actions, when adopted by communities around the world, help slow the spread of resistance and preserve the effectiveness of existing drugs.
A Call to Action: The Time to Act is Now
Antimicrobial resistance is a silent pandemic that’s already reshaping global health—and the clock is ticking. If left unchecked, it could undo decades of medical progress and endanger millions of lives each year.
But the crisis is not insurmountable. With coordinated efforts from governments, healthcare professionals, researchers, and the public, we can stop antimicrobial resistance in its tracks. Programs like those implemented by NNAST in Nigeria show that meaningful change is possible when strategy meets action.
Antimicrobial resistance may be a complex problem, but the solutions begin with awareness, education, and accountability. It’s up to all of us—globally and locally—to protect the future of medicine.